Sunday, May 7, 2017
FOODS BILL MARLER AND I DON’T EAT
As I was googling another food safety issue the other day, I came across the list of 6 foods that Bill Marler won’t eat. In case you don’t know who Bill Marler is, he is the most prominent food poisoning lawyer in the United States. He has made many millions of dollars representing victims of food poisoning. Clearly he has learned something along the way about the most risky foods to eat.
So here is his list (from http://www.foodpoisonjournal.com/food-poisoning-information/six-foods-bill-marler-never-eats). And then I will give you mine.
1. Unpasteurized (“raw”) milk and packaged (unpasteurized) juices.
2. Raw sprouts.
3. Meat that isn’t well done.
4. Prewashed or precut fruits and vegetables.
5. Raw or undercooked eggs.
6. Raw oysters and other raw shellfish.
Now, to my list. I avoid everything on Marler’s list with a few additions and modifications. The below refer to his above points.
1. Yes, absolutely.
2. Yes, again.
3. Yes, but I also avoid underdone chicken (but I imagine, if asked, Marler would agree).
4. I definitely avoid all precut fruits and vegetables, but I do on occasions eat bagged prewashed salads or greens such as spinach (after first rewashing them), though I prefer to eat the fruits, vegetables and herbs that I grow myself).
5. Absolutely agree.
6. Absolutely agree.
In addition, I avoid these foods:
1. Salsa (unless I make it myself).
2. Raw milk cheeses
3. Raw fish, including in ceviche and even sushi.
TSF
Monday, April 24, 2017
A BAD WEEK FOR POTATOES
We tend to think of potatoes as a relatively risk-free food. Offhand, how many cases of food poisoning can you think of in which potatoes have been involved? But the last few days may make us think twice about this popular vegetable.
McCain Foods USA, Inc. has had to recall their frozen hash brown potato products because of bits of golf balls (can you believe it?) hiding in them. I have been trying to figure out how on earth this could have happened. But I can see where it is possible. If a potato field happens to be near a golf course, a large mechanical harvester of potatoes could pick up a ball or two.
Anyway, throw out any 2 lb. bags of hash browns in your freezer if they are Roundy’s or Teeter brands, and if you live in Illinois and Wisconsin (Roundy’s brand) or in North Carolina, South Carolina, Virginia, District of Columbia, Delaware, Florida, Georgia and Maryland (Harris Teeter brand).
By the way, McCain Foods also supplies restaurants with vegetables and distributes to some 160 countries around the world. Who knows where golf-ball hash browns will pop up? You may want to be careful if you are biting into some hash browns at your favorite restaurant.
And you had better pass on the potato chips too if Jalapeño Flavored Frito-Lay‘s Kettle Cooked chips or Jalapeño Flavored Miss Vickie’s Kettle Cooked potato chips are your favorite. In this case there could be Salmonella bacteria in the Jalapeño seasoning that was used. Yes, as I discuss in The Safe Food Handbook (the book, not this blog) Salmonella bacteria are remarkably hardy. They can live in very dry conditions – as in spices – for months.
Remember, Salmonella can cause serious and sometimes fatal infections in young children, frail or elderly people, and anyone who has a weakened immune system, such as people receiving cancer treatment.
TSF
McCain Foods USA, Inc. has had to recall their frozen hash brown potato products because of bits of golf balls (can you believe it?) hiding in them. I have been trying to figure out how on earth this could have happened. But I can see where it is possible. If a potato field happens to be near a golf course, a large mechanical harvester of potatoes could pick up a ball or two.
Anyway, throw out any 2 lb. bags of hash browns in your freezer if they are Roundy’s or Teeter brands, and if you live in Illinois and Wisconsin (Roundy’s brand) or in North Carolina, South Carolina, Virginia, District of Columbia, Delaware, Florida, Georgia and Maryland (Harris Teeter brand).
By the way, McCain Foods also supplies restaurants with vegetables and distributes to some 160 countries around the world. Who knows where golf-ball hash browns will pop up? You may want to be careful if you are biting into some hash browns at your favorite restaurant.
And you had better pass on the potato chips too if Jalapeño Flavored Frito-Lay‘s Kettle Cooked chips or Jalapeño Flavored Miss Vickie’s Kettle Cooked potato chips are your favorite. In this case there could be Salmonella bacteria in the Jalapeño seasoning that was used. Yes, as I discuss in The Safe Food Handbook (the book, not this blog) Salmonella bacteria are remarkably hardy. They can live in very dry conditions – as in spices – for months.
Remember, Salmonella can cause serious and sometimes fatal infections in young children, frail or elderly people, and anyone who has a weakened immune system, such as people receiving cancer treatment.
TSF
Sunday, April 23, 2017
DOES PRESIDENT TRUMP EAT HASH BROWNS?
The chances are that President Trump will cut the budget of the FDA and USAID, which in turn will limit expenditure on keeping America's food safe.
In a way, it’s odd, because I would guess that Trump is at least very concerned about the safety of the food he personally eats. After all, he is a germaphope. He hates shaking hands, afraid that he will catch something. And one of the reasons he gives for eating junk food is that he claims big franchises are safer and more clean.
Of course, given that he eats his burgers and steaks well done, he should at least be able to avoid bacteria in meat unless there is cross contamination. And as far as we know, he doesn’t care much for vegetables except for potatoes.
But even cooked potatoes can sometimes carry risks. I wonder, for instance, whether he eats hash browns? If so, he had better be careful.
Today McCain Foods USA, Inc. issued a recall of widely distributed frozen hash brown products because they may be contaminated with golf ball materials. And some of these products were distributed in Florida where his “Winter White House” is located where he seems to be spending an inordinate amount of time - at taxpayer expense. If such hash brown potatoes are eaten, there is the risk of choking or injury to the mouth.
Of course, Trump is very keen on golf, but all the same, I doubt he is so keen he wants to eat the golf balls!
TSF
Thursday, April 13, 2017
IS TRUMP'S RESTAURANT ENCOURAGING FOOD POISONING?
Not good news for Trump’s “Winter White House.” Mar-a-Lago’s restaurant didn’t do well on the latest inspection on January 26. Inspectors found 13 health and sanitation code violations.
Is this a case of paying $200,000 membership fee for a nasty case of food poisoning? Maybe even worse if the victim is a visiting head of state being wined and dined there. Talk of embarrassing!
All U.S. restaurants are inspected on a regular basis by inspectors from local public health departments. There is some variation between how often they do it and what they look for, but usually it covers things like cleanliness of the kitchen area and food handling, cooking and storage procedures. They also try to make sure that food is not cross-contaminated or contaminated by employees or by cockroaches, flies or rodents running around. I checked out the actual list for Florida. It has fully 50 “high priority” categories on it, meaning that failure on any one of these could pose a risk of food poisoning for diners.
At Mar-a-Lago raw meat (chicken, duck, beef and ham) were stored at temperatures that were far too high for safety. What, they are now trying to save on their electricity bills? Or, was it because their refrigerators were not operating properly and needed repairs?
Also, it seems that the restaurant's fish that was to be served either raw or undercooked had not undergone proper inspection for parasites. If you have been reading the news or this blog about the recent unpleasant experience of two California newlyweds with rat lungworm disease (which they probably caught from food in Hawaii) you will know that parasites can be very nasty indeed.
Even some of the lesser violations at Mar-a-Lago (such as inadequate hand-washing facilities for employees) have been found to often lead to food poisoning. It seems that not only do they have paying for refrigerator repairs and for replacing rusting shelves, but also can’t afford to heat the water!
Maybe Trump should take a break from playing golf and go back to checking the kitchen himself. Apparently, when he used to do so in the past, Florida’s “Sanitation and Safety Specialists” (that is their proper name) cited Mar-a-Lago with far fewer violations. Or should he sent Ivanka down there? She seems to get things done.
TSF
Tuesday, April 11, 2017
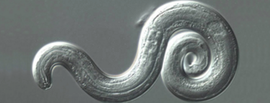
AVOID BRAIN INFECTING PARASITES
Ever heard of Angiostrongylus cantonensis? I bet you have now, even if you know it better as "rat lungworm disease." This brain infecting parasite was caught by two newlywed Californians while they were in Hawaii. Let’s face it, there is something thoroughly unpleasant about the idea of a worm crawling around in your brain. And, what’s more, according to the wife, it is very painful. And as evidenced by the experience of the husband, who spent a month in the ICU and is still hospitalized, the complications from this parasite can be very serious indeed.
So what are parasites? We've all heard of people being called "parasites." The chances are that you may have called your unemployed son a "parasite" at some point. A parasites is an organism that lives on or in a "host" organism and gets its food from it. In the process it can cause a lot of agony and damage to its host.
Parasitic diseases are most common in tropical, low-income countries, especially among the poorer people of those nations. I spent much of my professional life working in such areas, including on health and environmental problems affecting the poor. So guess what? Although I was very careful, I caught a number of parasites. I missed this one, thank goodness. Believe me, any parasite is not much fun at all.
So are we really at risk from them in countries like America and other industrialized nations? The answer is yes. A major reason is the increase in global travel, including to some pretty poor areas where in decades gone by, tourists generally did not go.
And yes, usually you get it from your food or water. In the case of the unlucky couple who are currently in the news, they probably caught the rat lungworm parasite from eating badly washed fruit or a vegetable such as lettuce, which carried this parasite-infected slug, a piece of the slug, or maybe just even just the slime of an infected slug. Or perhaps they got it from undercooked or raw crabs or freshwater shrimps.
What is the food safety lesson from this? Don’t eat raw vegetables (especially lettuce) while in tropical areas and make sure that any shellfish you eat is thoroughly cooked.
TSF
Wednesday, March 29, 2017
SENIORS ON CRUISES WATCH OUT!
I received sad news this morning. An elderly friend of mine had died. She became ill while on a cruise. The official cause will probably be listed as “congestive heart failure” or something similar. But although that explanation will be much more acceptable to the cruise line, it is not the whole story.
First, a bit of background. My friend is (I typed “is” as I am still having trouble using the past tense..)..was in her 80’s. Like many people of that age, she had a few chronic conditions, one being arthritis, and another, a “weak” heart. But she had never had a heart attack and her doctor in the UK considered her well enough to go on the cruise with her caregiver.
I was told that she really enjoyed the trip up until day 22 of this 44 day cruise. At that point there was an outbreak of food poisoning on the ship. She became very ill, dehydrated, and had to be sent to a hospital in Jamaica, which was the closest port. Several of the passengers ended up there, especially those who were over 60. At least one died soon after she was hospitalized in Jamaica.
Along with a few of the others, my friend was confined to the intensive care unit. After a few days she seemed to be better, but because she was still weak and considered at risk, she was sent to a hospital in Florida, and then to one in England, where she now lived. She died there.
If you have been following this blog, you will know that food poisoning outbreaks on cruise ships are common, with the majority of them caused by norovirus – a highly contagious group of viruses which often infects both passengers and crew. Usually an outbreak starts through contaminated food (perhaps contaminated by a crew member), but you can also catch it directly from someone who is ill (by taking care of them, using the same eating utensils or even from sprayed vomit), and, from surfaces.
Most people recover after 1-3 thoroughly miserable days. However, passengers who are older frequently develop severe dehydration which can aggravate or lead to other serious conditions as seemed to have occurred in my friend’s case. It is not unusual for relapses to happen a couple of weeks or so after the food poisoning incident itself, even after the patient seems to have recovered and has been released from hospital.
The Safe Food Handbook (available on Amazon) discusses how you can protect yourself, as do other posts on this blog. Be careful if you are going on a cruise!
TSF
Friday, March 24, 2017
IS SCHOOL LUNCH TOO DANGEROUS TO EAT?
I want to say right at the outset, that I believe in the value of school lunch. When I was a poor malnourished refugee child, I really appreciated that food. It is very hard to pay attention in class if you are hungry. But food poisoning outbreaks at schools are not unusual, simply because institutional food, prepared and served in bulk, is always more risky. And of course, such outbreaks get a lot of media coverage.
Recently there was a very large outbreak in Egypt caused by a school lunch (see earlier post), in which some 3,300 children had to be sent to hospital. In all, it is estimated that there have been 4,650 school lunch associated food poisoning cases nationwide in Egypt just this month (March, 2017). But Egypt is not the only country where such outbreaks occur. I have read case studies of school food poisoning outbreaks in India, Canada, UK, Japan and elsewhere. How the school lunch is organized and how sanitary the conditions are, varies in these and other countries.
In the United States, the National School Lunch Program is carefully supervised, but even then, food poisoning outbreaks occur. It is estimated that between 1991 and 2000 (I don’t have later statistics) there were 300 outbreaks of food poisoning in American schools, which made at least 16,000 students ill. The largest during that decade affected school children in seven states in 1997-1998. It was unusual in that it was caused by a toxic mold in frozen burritos.
But there have been many different types of causes over the years. Bacteria such as Salmonella, E.coli and Staphylococcus strains have been found to cause food poisoning in school lunches. Even agricultural chemicals have been involved, though less than they are in Third World countries. Several incidents have of course been caused by the common norovirus. That was the cause of the recent outbreak of food poisoning at the St. Charles East High School in Illinois, USA, in which some 800 students became ill.
As of this past Wednesday, the Ministry of Education in Egypt suspended school lunches, which feed some 9 million students a day. It plans to set up a committee (the usual bureaucratic solution) and conduct an investigation of why school lunches are so unsafe. I can hazard a few guesses.
TSF
Subscribe to:
Posts (Atom)